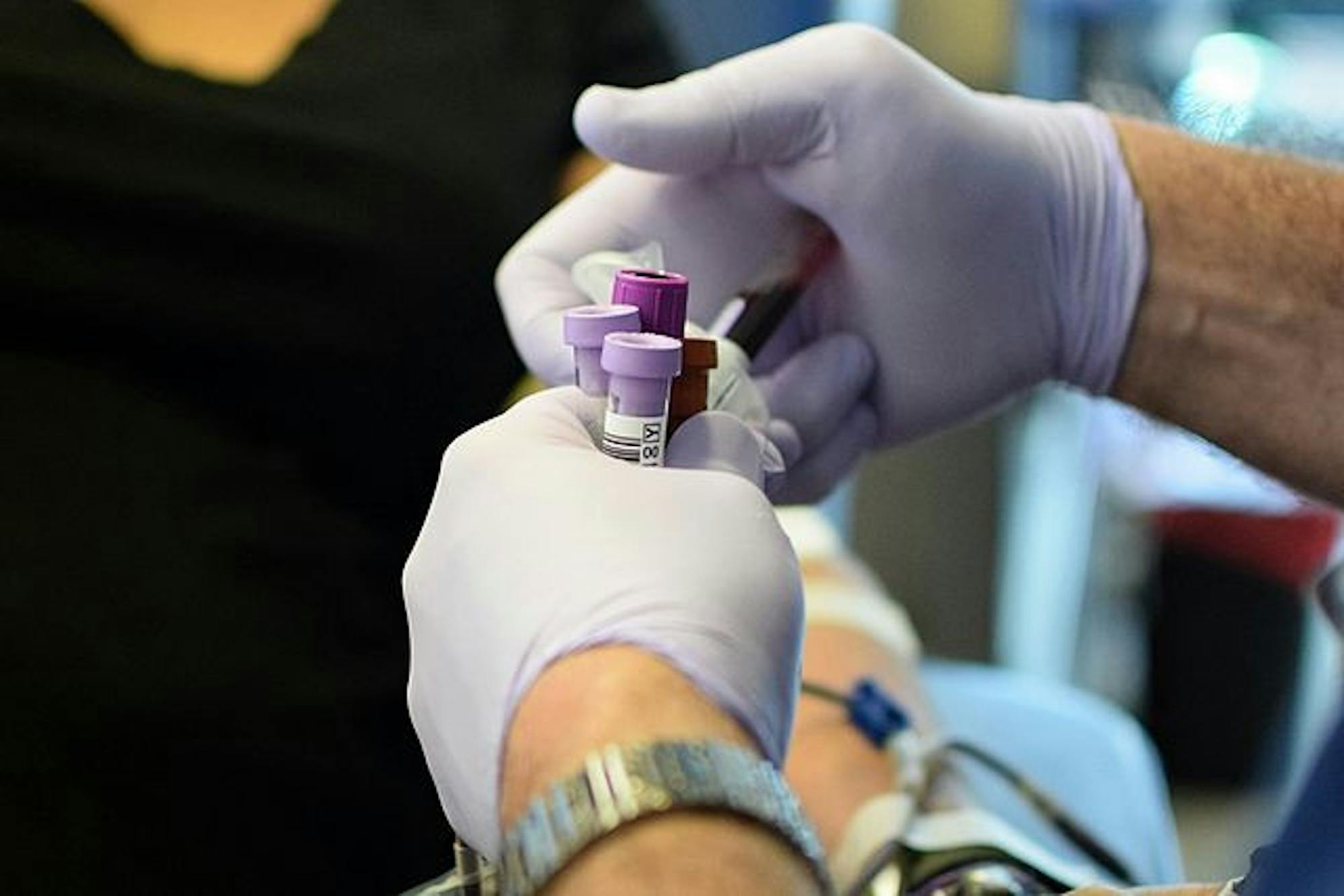
Donating blood — it’s a simple act that can save a life, or several. Yet, current Food and Drug Administration regulations require that gay and bisexual men only donate blood under the condition that they have not engaged in sexual intercourse with another man for the past three months. This restriction, a product of the 1980s AIDS crisis, precedes the widespread research and education regarding the AIDS and HIV now available. This outdated policy has drastically reduced the amount of possible blood donors across the United States, along with the number of possible lives that could be saved.
In January, a series of new draft recommendations released by the FDA proposed a shift from time-based restrictions to alternative donor deferral policies using gender-inclusive, individualized questions to reduce the risk of transfusion-transmitted HIV. This is a groundbreaking step in the right direction, as these proposals not only aim to foster inclusivity but also address a need for more blood. The United States has been experiencing its worst blood shortage in over a decade, and there are people desperately in need of transfusions to survive.
The FDA has also implemented rules stating that those who are currently on medication to prevent HIV or those who have recently had sex in exchange for money or drugs would be subject to the three-month deferral period. This restriction is in an effort to protect the quality of blood in the United States, regardless of sexual or gender orientation. Still, this new proposal would have a significant impact on the shortages in blood supply in the United States. Projected statistics show that if the blood donor bans were lifted for gay and bisexual men, the annual blood supply would expand by 345,400–615,300 pints of blood.
The FDA is expected to make their final decision following a 60-day public comment period. Many argue that this new proposal, more than 40 years in the making for LGBTQ+ advocacy organizations and other public health institutions, does not go far enough. Some believe that these restrictions still promote an unnecessary stigma against those taking PrEP medication to prevent HIV and that the blood supply shortage does not stem from HIV-infected blood but rather a lack of donors in the first place. After all, the blood-supply crisis in the United States isn’t about the quality of the blood — it’s the fact that there simply isn’t enough of it.